Understanding the Causes of Bedsores and Pressure Injuries
Bedsores, also known as pressure ulcers or pressure injuries, develop when sustained pressure damages skin and underlying tissue. Understanding what causes these injuries helps explain why they are considered preventable—and why their development in healthcare settings often indicates a failure to provide proper care.
What Causes Bedsores?
Bedsores develop when blood flow to an area of skin is reduced or cut off, usually due to sustained pressure against the tissue. Without adequate blood flow, skin cells and underlying tissues are deprived of oxygen and nutrients, causing them to break down and die. This damage can occur surprisingly quickly—sometimes within hours—in vulnerable patients.
While pressure is the primary cause, several factors contribute to bedsore development. Understanding these causes helps explain why certain patients are at higher risk and why proper care protocols are essential for prevention.
Sustained Pressure: The Primary Cause
Pressure is the fundamental cause of bedsores. When skin and tissue are compressed between a bone and an external surface (such as a mattress, wheelchair cushion, or chair), blood vessels are squeezed shut. This prevents blood from delivering oxygen and nutrients to the affected tissue.
Research shows that tissue damage can begin within 1-2 hours of sustained pressure in high-risk patients. This is why healthcare facilities are required to reposition immobile patients at regular intervals—typically every 2 hours for bed-bound patients and every 15-30 minutes for those in wheelchairs.
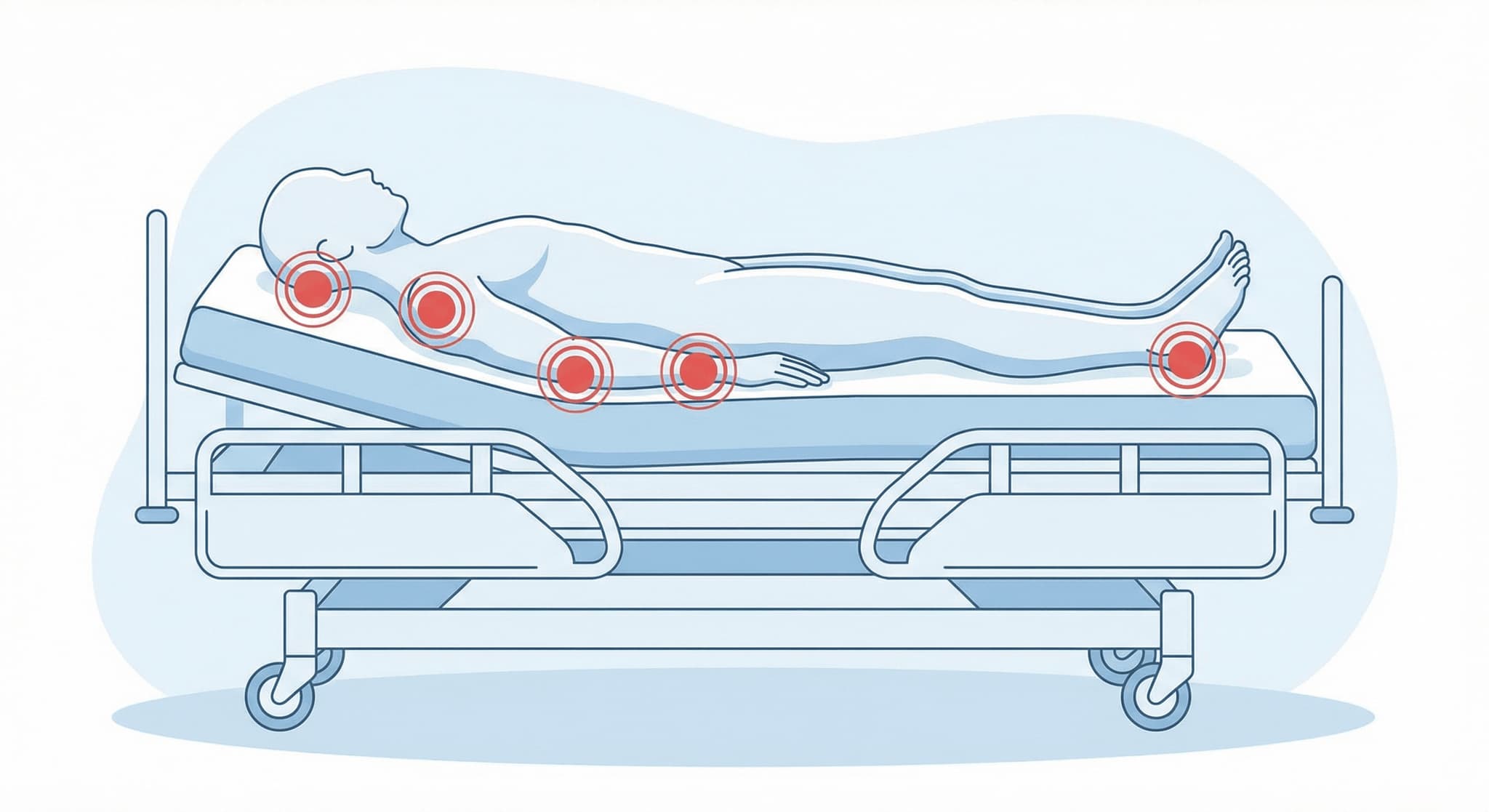
High-Risk Pressure Points
Bedsores most commonly develop over bony prominences where there is little padding between skin and bone:
- Sacrum and tailbone: The most common location, especially for patients lying on their backs
- Heels: Extremely vulnerable due to thin skin and minimal soft tissue
- Hips (trochanter): At risk when patients lie on their side
- Ischial tuberosities: The "sit bones" affected by wheelchair use
- Shoulder blades and elbows: Contact points when lying on the back
- Back of the head: Particularly vulnerable in patients who cannot move their heads
- Ears: At risk from oxygen tubing and positioning devices
Friction: Surface Damage to Skin
Friction occurs when skin rubs against another surface, such as bed linens, clothing, or medical equipment. This rubbing action can damage the outer layer of skin (epidermis), making it more vulnerable to breakdown.
Friction injuries commonly occur when:
- Patients are dragged rather than lifted during transfers or repositioning
- Bed linens are pulled out from under a patient instead of properly changed
- Patients slide down in bed or in a wheelchair
- Agitated patients move repeatedly against sheets or restraints
Proper transfer techniques—using lift sheets, slide boards, and adequate staff—can prevent friction injuries. When healthcare staff drag patients rather than lift them properly, they are not following established care standards.
Shear: Hidden Tissue Damage
Shear is a particularly damaging force that occurs when skin moves in one direction while underlying tissue moves in another. This creates stretching and tearing of blood vessels beneath the skin surface.
The most common scenario for shear injury is when a patient slides down in bed while the head of the bed is elevated. The skin on the sacrum may stay in place (held by friction against the mattress) while the skeleton and deeper tissues slide downward. This stretches and damages the blood vessels in between, reducing blood flow to the tissue.
Shear is dangerous because the damage occurs internally, beneath skin that may initially appear intact. This can lead to deep tissue injuries that become apparent only after significant damage has occurred.
Preventing Shear Injuries
- Limiting the angle of bed elevation to 30 degrees or less when possible
- Using proper positioning devices to prevent sliding
- Repositioning patients after raising the head of the bed
- Ensuring patients are properly positioned in wheelchairs with footrests at the correct height
Moisture: Weakening the Skin's Defenses
Moisture makes skin more vulnerable to damage from pressure, friction, and shear. When skin is wet, it becomes softer and more easily damaged. Prolonged moisture exposure can lead to maceration—a condition where skin becomes pale, wrinkled, and fragile.
Common sources of moisture that increase bedsore risk include:
- Urinary incontinence: Urine is particularly damaging due to its chemical composition, which can irritate and break down skin
- Fecal incontinence: Contains bacteria and enzymes that rapidly damage skin; even more harmful than urine
- Perspiration: Can accumulate in skin folds and areas of contact
- Wound drainage: Leakage from existing wounds can damage surrounding skin
Moisture Management in Healthcare Settings
Proper moisture management is a fundamental aspect of pressure injury prevention. Healthcare facilities should:
- Implement scheduled toileting programs for incontinent patients
- Change soiled briefs and linens promptly
- Apply barrier creams to protect skin from moisture
- Use moisture-wicking linens and absorbent underpads
- Document incontinence episodes and skin checks
When patients are left in soiled briefs for extended periods, the facility is failing to meet basic care standards.
Immobility: The Underlying Risk Factor
Healthy individuals constantly make small movements, even during sleep, that relieve pressure on vulnerable areas. We shift position when we feel discomfort, preventing any single area from being compressed for too long. This natural protective mechanism is impaired or absent in many healthcare patients.
Conditions and situations that cause immobility include:
- Paralysis or spinal cord injury: Inability to feel or respond to pressure discomfort
- Sedation or anesthesia: Surgical patients are at high risk during and after procedures
- Stroke: May affect ability to move or sense pressure on one side
- Advanced dementia: May not recognize or respond to discomfort signals
- Severe illness or weakness: Lack of strength to reposition oneself
- Coma or unconsciousness: Complete inability to move independently
- Physical restraints: Limit ability to shift position
- Pain or contractures: May limit the positions a patient can tolerate
When patients cannot reposition themselves, the responsibility falls entirely on healthcare providers. Regular repositioning schedules, pressure-redistributing mattresses, and careful monitoring are essential.
Poor Nutrition and Dehydration
Adequate nutrition plays a crucial role in maintaining skin integrity and supporting tissue healing. Patients who are malnourished or dehydrated have skin that is more fragile and more susceptible to pressure damage. They also have reduced ability to heal any injuries that do occur.
Key Nutritional Factors
- Protein: Essential for skin maintenance and wound healing. Low protein levels (hypoalbuminemia) significantly increase bedsore risk.
- Calories: Inadequate caloric intake leads to muscle wasting, reducing the natural padding over bony prominences.
- Hydration: Dehydrated skin is less elastic and more vulnerable to damage.
- Vitamins and minerals: Vitamin C and zinc are particularly important for skin health and wound healing.
Nutritional Care in Healthcare Settings
Healthcare facilities are required to assess patients' nutritional status and provide adequate nutrition. This includes:
- Conducting nutritional assessments upon admission and regularly thereafter
- Monitoring food and fluid intake
- Providing assistance with eating when needed
- Consulting dietitians for patients at nutritional risk
- Considering nutritional supplements when dietary intake is inadequate
Weight loss and signs of malnutrition in a healthcare setting should trigger immediate intervention. Allowing a patient's nutritional status to deteriorate represents a failure of care.
Additional Risk Factors
Beyond the direct causes of bedsores, several additional factors increase a patient's vulnerability:
- Advanced age: Aging skin is thinner, drier, and less elastic
- Poor circulation: Reduces blood flow to extremities and skin
- Diabetes: Affects circulation and sensation, particularly in lower extremities
- Peripheral vascular disease: Compromises blood supply to tissues
- Previous pressure injuries: Scar tissue is more vulnerable to breakdown
- Smoking: Impairs circulation and tissue oxygenation
- Low blood pressure: Reduces perfusion to skin and tissues
- Certain medications: Sedatives and pain medications can reduce mobility
Why Bedsores Are Preventable
The causes of bedsores are well understood, and effective prevention strategies exist. Medical literature and regulatory guidelines are clear: with proper care, the vast majority of bedsores can be prevented.
Prevention requires:
- Risk assessment: Identifying patients at risk using validated tools (like the Braden Scale)
- Repositioning: Regular turning of immobile patients, typically every 2 hours
- Pressure redistribution: Using appropriate mattresses, cushions, and support surfaces
- Skin care: Keeping skin clean, dry, and moisturized
- Moisture management: Promptly addressing incontinence and perspiration
- Nutrition: Ensuring adequate protein, calories, and hydration
- Proper techniques: Using correct methods for lifting and transferring patients
- Documentation: Recording skin assessments and prevention activities
When bedsores develop in hospitals, nursing homes, or other healthcare facilities, it often indicates that one or more of these prevention measures was not properly implemented. Understanding the causes helps identify where care may have fallen short.
When Development Indicates Negligence
Because bedsores are largely preventable with proper care, their development in a healthcare setting often raises questions about the quality of care provided. Consider consulting with an attorney if:
- Your loved one developed new bedsores while in a healthcare facility
- An existing bedsore worsened or progressed to a more severe stage
- The facility did not inform you about the bedsore promptly
- You observed signs of inadequate care (infrequent repositioning, wet linens, weight loss)
- Bedsores led to complications such as infection, sepsis, or hospitalization
At Traction Law Group, we review medical records to understand how bedsores developed and whether proper prevention protocols were followed. Learn more about bedsore lawsuits or contact us for a free consultation.
Additional Resources
For more information about bedsores and pressure injuries, explore these related guides:
- Understanding Pressure Ulcer Stages – Learn how bedsores are classified and why staging matters
- What To Do If Your Loved One Has Bedsores – Immediate steps and guidance for concerned families
- How to Document Bedsores – Tips for photographing and recording evidence
- Bedsore Complications – Serious conditions that can develop from untreated bedsores
Sources & References
- Pressure Injury Stages and Prevention — National Pressure Injury Advisory Panel (NPIAP). Accessed January 2026.
- Pressure Ulcer Prevention and Treatment Clinical Practice Guidelines — Agency for Healthcare Research and Quality (AHRQ). Accessed January 2026.
- Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline — European Pressure Ulcer Advisory Panel (EPUAP). Accessed January 2026.
- State Operations Manual: Guidance for Surveyors in Long-Term Care — Centers for Medicare & Medicaid Services (CMS). Accessed January 2026.
Concerned About a Loved One's Bedsore?
If your loved one developed bedsores in a healthcare facility, the injury may have been preventable. Contact us for a free, confidential consultation to understand your options.
Related Conditions & Topics
Understanding Pressure Ulcer Stages
Learn about the different stages of pressure injuries and how they progress.
Learn MoreStage 1 Pressure Ulcers
Early warning signs of bedsores and why prompt intervention matters.
Learn MoreBedsore Infections
How untreated bedsores can become infected and lead to serious complications.
Learn MoreBedsore Prevention Standards
How healthcare facilities should prevent pressure injuries from developing.
Learn MoreNursing Home Bedsore Lawyer
Legal options when facility negligence allows preventable bedsores to develop.
Learn MoreGet Your Free Case Evaluation
Fill out the form below and our team will review your case immediately.