Stage 1 Pressure Ulcer
Stage 1 pressure ulcers are the earliest warning sign of tissue damage. Though the skin remains intact, this stage demands immediate attention—failure to act can lead to rapid deterioration and more serious wounds.
What Is a Stage 1 Pressure Ulcer?
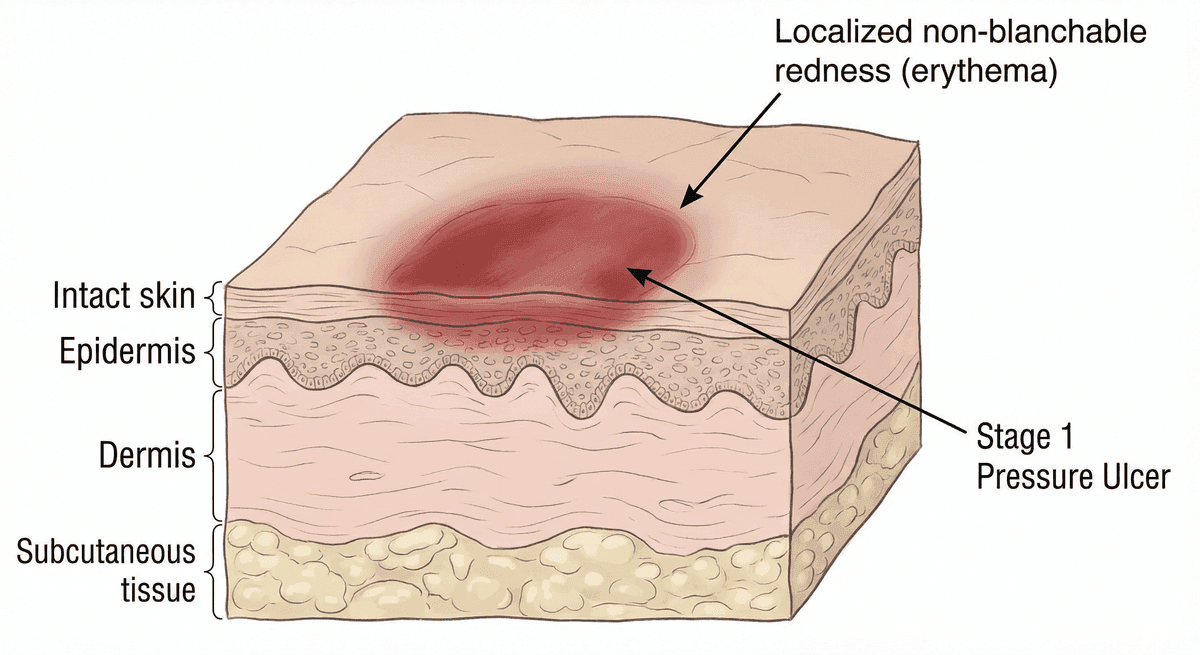
A Stage 1 pressure ulcer represents the earliest identifiable stage of pressure-related skin damage. According to the National Pressure Injury Advisory Panel (NPIAP), Stage 1 is defined as intact skin with a localized area of non-blanchable erythema, typically over a bony prominence. In individuals with darker skin tones, the redness may be more difficult to detect, but the area may appear a different color than surrounding tissue.
The key distinguishing feature of a Stage 1 ulcer is that the skin remains unbroken. Unlike more advanced stages, there is no open wound, blister, or visible tissue damage. However, the underlying tissue has already begun to suffer from inadequate blood flow and oxygen, making prompt intervention necessary.
How to Identify Stage 1 Pressure Ulcers
Recognizing a Stage 1 pressure ulcer requires careful skin assessment. Healthcare providers in nursing homes and hospitals should perform regular skin checks specifically designed to identify these early warning signs.
The Blanching Test
The primary method for identifying Stage 1 ulcers is the blanching test. When you press on healthy skin, it temporarily turns white (blanches) as blood is pushed from the capillaries, then quickly returns to its normal color when pressure is released. In Stage 1 pressure ulcers, the affected area does not blanch—it remains red or discolored even when pressed. This non-blanchable erythema indicates that the underlying blood vessels have been damaged.
Visual Signs
- Persistent redness that does not fade within 30 minutes after pressure is relieved
- In darker skin tones: purple, blue, or ashen discoloration
- Color that differs noticeably from surrounding skin
- The affected area may appear shiny or taut
Sensory Changes
- The area may feel warmer or cooler than surrounding tissue
- The patient may report pain, burning, or itching at the site
- The tissue may feel firmer (indurated) or softer (boggy) than normal
- Some patients may report numbness or tingling
Common Locations
Stage 1 pressure ulcers most frequently develop over bony prominences where the body's weight creates pressure against the skin. The location often depends on the patient's typical position:
- For patients lying on their back: sacrum (tailbone), heels, shoulder blades, back of the head
- For patients lying on their side: hips (greater trochanter), ankles, knees, ears, shoulders
- For patients in wheelchairs: ischial tuberosities (sitting bones), tailbone, shoulder blades
Proper skin assessments should check all vulnerable areas based on the patient's position and mobility level.
Causes and Risk Factors
Stage 1 pressure ulcers develop when sustained pressure on the skin restricts blood flow to the underlying tissue. Without adequate oxygen and nutrients, the tissue begins to break down. Several factors increase the risk:
Primary Causes
- Immobility: Patients who cannot reposition themselves independently are at highest risk
- Prolonged pressure: Remaining in the same position for extended periods without repositioning
- Friction: Skin rubbing against bedding or wheelchair surfaces
- Shear: Layers of skin moving in opposite directions, often when sliding down in bed
Contributing Risk Factors
- Advanced age and fragile skin
- Poor nutrition or dehydration
- Incontinence (moisture weakens skin integrity)
- Reduced sensation (from diabetes, stroke, or spinal cord injury)
- Poor circulation or cardiovascular disease
- Low body weight or obesity
- Cognitive impairment or inability to communicate discomfort
Prevention at This Stage
The appearance of a Stage 1 pressure ulcer is a warning that demands immediate preventive action. When identified and addressed promptly, Stage 1 ulcers are fully reversible. Prevention strategies include:
Pressure Relief
- Immediately relieve pressure from the affected area
- Reposition the patient at least every two hours (or more frequently if needed)
- Use pressure-redistributing mattresses and cushions
- Keep heels elevated off the bed using pillows or specialized heel protectors
- Avoid positioning the patient directly on the affected area until it has healed
Skin Care
- Keep skin clean and dry
- Manage incontinence promptly with appropriate products
- Apply moisturizers to prevent dry skin from cracking
- Avoid massage over reddened areas (this can cause additional damage)
- Use protective dressings or barrier creams as directed
Nutrition and Hydration
- Ensure adequate protein intake to support tissue health
- Maintain proper hydration
- Consider nutritional supplements if the patient is at risk for malnutrition
What Happens Without Treatment
Without proper intervention, Stage 1 pressure ulcers can rapidly progress to more severe stages. The skin may break down within hours or days, leading to:
- Stage 2: Partial thickness skin loss with exposed dermis, often appearing as a shallow open wound or blister
- Stage 3: Full thickness skin loss with visible fat tissue but no exposed bone, tendon, or muscle
- Stage 4: Full thickness tissue loss with exposed bone, tendon, or muscle—a serious wound that may require surgery
Advanced pressure ulcers are much more difficult to treat, carry a significant risk of infection and sepsis, and in severe cases can be life-threatening.
Standard of Care Requirements
Healthcare facilities have a legal and ethical duty to prevent pressure ulcers. For Stage 1 injuries specifically, the standard of care requires:
- Regular skin assessments upon admission and at least daily thereafter for at-risk patients
- Immediate documentation when Stage 1 changes are observed
- Prompt implementation of a pressure injury prevention care plan
- Notification of the physician or wound care team
- Patient and family education about the condition
- Ongoing monitoring to ensure the condition improves, not worsens
When facilities fail to follow these protocols, and a Stage 1 ulcer progresses to a more serious wound, negligence may be a factor. Learn more about bedsore prevention standards that facilities are required to follow.
When to Seek Legal Help
While Stage 1 pressure ulcers can heal quickly with appropriate care, their presence often indicates larger problems with facility care. You may want to consult an attorney if:
- A Stage 1 ulcer was not identified despite regular assessments being required
- The facility failed to implement preventive measures once Stage 1 was identified
- The ulcer progressed to Stage 2, 3, or 4 due to inadequate care
- Your loved one developed multiple pressure ulcers at different sites
- Staff seemed unaware of the wound or dismissed your concerns
- Documentation of skin assessments or repositioning is missing or incomplete
Stage 1 ulcers that progress to more severe wounds often indicate systemic failures in care—understaffing, inadequate training, or corporate cost-cutting. At Traction Law Group, we help families understand their legal options and hold negligent facilities accountable. Contact a nursing home bedsore lawyer or find an attorney in your area through our state bedsore lawyer directory.
Documenting Stage 1 Concerns
If you notice signs of a Stage 1 pressure ulcer on your loved one, take these steps:
- Photograph the affected area with a timestamp if possible, including comparison to surrounding skin
- Note the location and describe what you observe (color, warmth, firmness)
- Ask staff what they know about the condition and document their response
- Request the care plan to see what prevention measures are in place
- Monitor for changes at each visit and continue documenting
This documentation can be valuable if the condition worsens and you need to demonstrate that earlier warning signs were present but not properly addressed. For more guidance, see our resource on how to document bedsores.
Frequently Asked Questions
- Q. What does a Stage 1 pressure ulcer look like?
- A Stage 1 pressure ulcer appears as a localized area of non-blanchable redness on intact skin, typically over a bony prominence. The skin does not break or open. In patients with darker skin tones, the area may appear purple, blue, or ashen rather than red. The affected area may also feel warmer, cooler, firmer, or softer than surrounding tissue.
- Q. Can Stage 1 bedsores heal on their own?
- Stage 1 pressure ulcers can heal within a few days when pressure is relieved and proper care is provided, including repositioning every two hours, using pressure-redistributing surfaces, and maintaining good nutrition. However, without intervention, Stage 1 ulcers will not resolve and will likely progress to more serious stages. According to AHRQ guidelines, prompt identification and treatment at this stage is critical.
- Q. Is a Stage 1 bedsore a sign of nursing home neglect?
- A Stage 1 bedsore can indicate inadequate care, especially if the facility failed to conduct regular skin assessments, implement repositioning schedules, or address known risk factors. While not every Stage 1 ulcer results from neglect, a pattern of pressure injuries or progression to more severe stages often points to systemic care deficiencies. Families concerned about a loved one's care should document the condition and consult with a bedsore attorney.
- Q. How quickly can Stage 1 pressure ulcers develop?
- Stage 1 pressure ulcers can develop within hours of sustained, unrelieved pressure on the skin. Patients who are immobile, malnourished, or incontinent are at the highest risk. According to the National Pressure Injury Advisory Panel (NPIAP), regular skin assessments and repositioning at least every two hours are essential to prevent pressure injuries from forming.
- Q. What should I do if my loved one has a Stage 1 bedsore in a nursing home?
- If you notice signs of a Stage 1 pressure ulcer, photograph the area with a timestamp, ask staff about the care plan and repositioning schedule, request copies of skin assessment records, and monitor the area during each visit. If the wound worsens or you suspect inadequate care, contact Traction Law Group for a free consultation to understand your legal options.
Sources & References
- Pressure Ulcer Stages Revised by NPUAP — National Pressure Ulcer Advisory Panel (now NPIAP). Accessed January 2026.
- Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline — European Pressure Ulcer Advisory Panel, NPIAP, and Pan Pacific Pressure Injury Alliance. Accessed January 2026.
- Pressure Ulcers (Pressure Injuries) and Wound Care — Agency for Healthcare Research and Quality (AHRQ). Accessed January 2026.
- MDS 3.0 Quality Measures User Manual — Centers for Medicare & Medicaid Services (CMS). Accessed January 2026.
Concerned About a Loved One's Care?
If your family member developed a Stage 1 pressure ulcer that was ignored or progressed to a more severe wound, negligence may be a factor. Contact us for a free consultation.
Related Conditions & Topics
Stage 2 Pressure Ulcer
When Stage 1 progresses to partial thickness skin loss.
Learn MoreAll Pressure Ulcer Stages
Overview of all pressure injury stages and classifications.
Learn MoreBedsore Infection
Understanding infection risks in pressure ulcers.
Learn MoreNursing Home Bedsore Lawyer
Legal options when bedsores develop in nursing homes.
Learn MoreGet Your Free Case Evaluation
Fill out the form below and our team will review your case immediately.