Hospital-Acquired Pressure Injury Lawyer
When hospitals fail to prevent bedsores in their care, patients suffer needless harm. We help patients and families hold hospitals accountable for pressure injuries that should never have occurred.
Understanding Hospital-Acquired Pressure Injuries
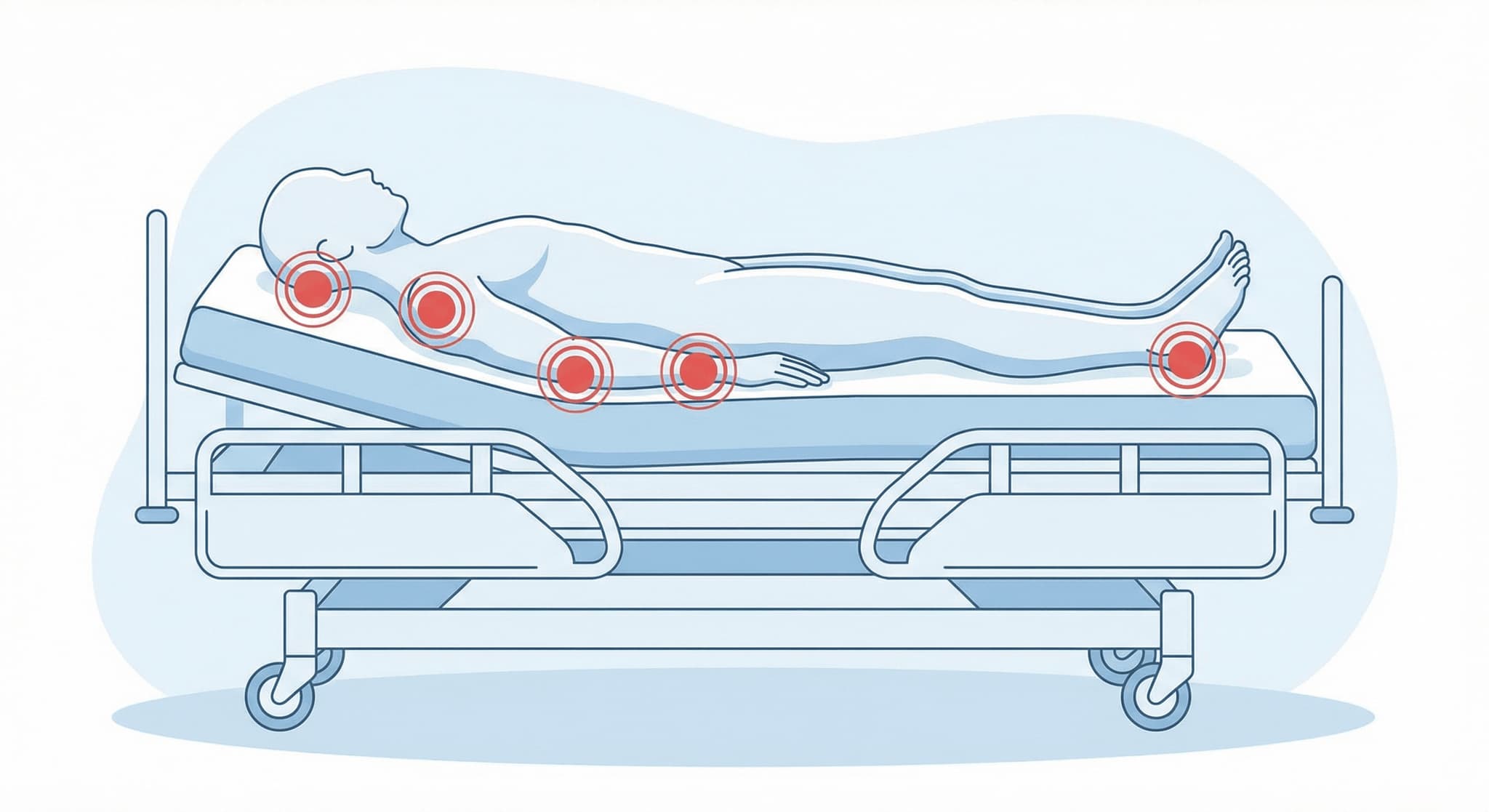
Hospital-acquired pressure injuries (HAPIs) are bedsores that develop during a patient's hospital stay. These wounds form when sustained pressure on the skin—typically over bony areas like the tailbone, heels, and hips—cuts off blood flow and causes tissue damage. While any hospitalized patient can develop a pressure injury, those who are critically ill, undergoing surgery, or unable to move independently face the highest risk.
Major healthcare organizations, including the Centers for Medicare and Medicaid Services (CMS), classify hospital-acquired pressure ulcers as "never events"—serious, largely preventable errors that should not occur if proper care protocols are followed. Despite this designation, thousands of patients develop HAPIs each year, often resulting in extended hospital stays, additional surgeries, serious infections, and in some cases, death.
Hospital Standard of Care
Hospitals are required to meet established standards of care for pressure injury prevention. These standards are based on evidence-based guidelines and include:
- Risk Assessment on Admission: Every patient should be evaluated for pressure injury risk using standardized tools like the Braden Scale, which measures factors including mobility, nutrition, and skin moisture.
- Prevention Care Plans: High-risk patients require individualized prevention plans that address their specific risk factors.
- Regular Repositioning: Immobile patients must be turned and repositioned at least every two hours to relieve pressure on vulnerable areas.
- Pressure-Relieving Surfaces: Appropriate mattresses, overlays, and heel protectors should be provided to at-risk patients.
- Skin Assessments: Nursing staff should conduct regular skin checks and document any changes in condition.
- Nutrition and Hydration: Adequate nutrition is essential for skin integrity; patients at risk should receive nutritional support.
- Documentation: All assessments, interventions, and skin changes must be thoroughly documented in the medical record.
When hospitals fail to implement these measures and patients develop pressure injuries as a result, the facility may be liable for medical malpractice.
Why Bedsores Develop in Hospitals
Hospital patients face unique risk factors that make pressure injury prevention both more important and more challenging:
Limited Mobility
Patients recovering from surgery, illness, or injury often cannot move independently. Those on bed rest, connected to medical equipment, or experiencing pain may remain in one position for hours without the ability to shift their weight.
Sedation and Anesthesia
Patients under sedation or general anesthesia cannot feel pressure discomfort that would normally prompt them to move. This makes them entirely dependent on hospital staff for repositioning.
Medical Devices
Oxygen masks, catheters, IV lines, and other medical devices can create pressure points that lead to device-related pressure injuries. These must be regularly repositioned and the underlying skin monitored.
Underlying Conditions
Patients with diabetes, vascular disease, or compromised circulation face increased risk. However, hospitals are expected to identify these risk factors and implement appropriate prevention measures.
Staffing and Workload
When units are understaffed or nurses have excessive patient loads, time-intensive tasks like repositioning may be delayed or skipped. Budget constraints should never compromise patient safety.
ICU and Surgical Patient Risks
Intensive care unit patients and those undergoing long surgical procedures face particularly elevated risks for hospital-acquired pressure injuries.
ICU Patients
Critical care patients are often sedated, on mechanical ventilation, and connected to multiple medical devices. They may be hemodynamically unstable, making repositioning complicated but not impossible. ICU nursing protocols should account for these challenges with specialized approaches to pressure injury prevention.
Common ICU-related pressure injuries occur on the:
- Sacrum and coccyx (tailbone) from prolonged supine positioning
- Heels from contact with the bed surface
- Occiput (back of the head) from immobility
- Face and nose from oxygen masks and tubes
- Ears from medical tubing
Surgical Patients
Patients undergoing lengthy surgical procedures may remain in one position on the operating table for hours. While the surgical team focuses on the procedure, pressure builds on dependent body surfaces. Pre- and post-operative skin assessments, appropriate positioning pads, and post-surgical monitoring are essential prevention measures.
Operating room-acquired pressure injuries may not become apparent until 24-72 hours after surgery, when tissue damage from sustained pressure becomes visible. This delayed presentation can make it harder to identify the cause, but medical records should document positioning and preventive measures used during the procedure.
Holding Hospitals Accountable
Hospital-acquired pressure injuries represent a failure of care. While hospitals may argue that some patients develop bedsores despite best efforts, the evidence often reveals gaps in prevention protocols, missed assessments, or inadequate staffing.
Key evidence in hospital pressure injury cases includes:
- Admission Assessments: Was the patient's pressure injury risk properly evaluated? Were appropriate interventions ordered?
- Turning and Repositioning Records: Did staff document regular repositioning? Are there gaps in the turning schedule?
- Skin Assessment Documentation: Were skin checks performed and documented? When was the first sign of skin breakdown noted?
- Nursing Notes: What do nursing observations reveal about the patient's condition and care provided?
- Staffing Records: Was the unit adequately staffed to provide required care?
- Photographs: Images showing the location, staging, and progression of the wound.
We work with medical professionals to review hospital records, identify deviations from the standard of care, and build cases that demonstrate how the hospital's failures led to preventable harm.
Your Legal Options
If you or a loved one developed a hospital-acquired pressure injury due to negligent care, you may be able to pursue compensation for:
- Additional medical treatment required for the pressure injury
- Extended hospital stays and rehabilitation
- Pain and suffering caused by the wound
- Permanent scarring or disfigurement
- Lost wages if the injury delayed your return to work
- Complications such as infection or sepsis resulting from the pressure injury
- Wrongful death if complications proved fatal
We represent patients and families across the country in hospital negligence cases. Our team understands the medical complexity of these injuries and the legal strategies needed to hold large healthcare institutions accountable.
How We Help
At Traction Law Group, we represent patients and families who have been harmed by hospital negligence. Our approach includes:
- Free Case Evaluation: We review your medical records and circumstances at no cost to determine if you have a viable claim.
- Medical Record Analysis: We obtain complete hospital records and work with healthcare professionals to identify where the standard of care was breached.
- No Upfront Costs: We work on contingency—you pay nothing unless we recover compensation on your behalf.
- National Representation: We help patients and families throughout the United States pursue justice against negligent hospitals.
Hospitals have legal teams and insurance companies working to protect their interests. You deserve someone fighting for yours.
Frequently Asked Questions
- Q.What is a hospital-acquired pressure injury (HAPI)?
- A hospital-acquired pressure injury is a bedsore or pressure ulcer that develops during a hospital stay. These injuries typically occur when patients remain in one position for extended periods without proper repositioning, especially in intensive care units or during long surgeries. HAPIs are considered a "never event" by healthcare quality organizations because they are largely preventable with proper care.
- Q.Are hospitals always responsible for bedsores that develop during a stay?
- Not automatically, but hospitals have a duty to assess patient risk, implement prevention protocols, and monitor skin condition. When they fail to take reasonable preventive measures and a patient develops a pressure injury as a result, the hospital may be liable. Each case depends on the specific circumstances and whether the standard of care was met.
- Q.Why do bedsores develop in hospitals?
- Hospital patients are at elevated risk for several reasons: limited mobility during recovery, sedation or anesthesia preventing movement, extended time on operating tables, use of medical devices that create pressure points, and staff focused on treating the primary condition rather than skin care. While these factors increase risk, hospitals are expected to account for them in their prevention protocols.
- Q.How quickly can bedsores develop in a hospital?
- Pressure injuries can begin forming in as little as 2-4 hours of unrelieved pressure. This is why regular repositioning and skin checks are so important. Patients in surgery or on ventilators may be immobile for extended periods, making vigilant prevention essential.
- Q.Can I sue a hospital for a bedsore my family member developed during surgery?
- You may have a claim if the hospital failed to take appropriate precautions before, during, or after surgery. Long surgical procedures carry inherent risks, but hospitals are expected to use pressure-relieving positioning, conduct skin assessments, and provide post-operative monitoring. An attorney can evaluate whether the standard of care was breached.
- Q.What should I do if I notice a bedsore developing during a hospital stay?
- Immediately notify the nursing staff and attending physician. Request that they document the wound in the medical record. Take photographs if possible. Ask what prevention measures were in place and what treatment will be provided. Request copies of the medical records when discharged. If the injury is serious, consider consulting an attorney to understand your options.
- Q.What compensation is available for hospital-acquired pressure injuries?
- Patients who develop HAPIs due to hospital negligence may recover compensation for additional medical treatment, extended hospital stays, pain and suffering, permanent scarring or disfigurement, and in severe cases, complications like infection or sepsis. The specific damages depend on the severity of the injury and its impact on the patient.
You Trusted the Hospital With Your Care
If you or a loved one developed bedsores during a hospital stay, you may have legal options. Contact us for a free, confidential consultation.
Related Information
National Bedsore Lawyers
Overview of bedsore litigation and how we help patients and families.
Learn MoreNursing Home Bedsore Lawyer
Legal options when bedsores develop in long-term care facilities.
Learn MoreWrongful Death from Bedsores
Information for families who lost loved ones to bedsore complications.
Learn MoreBedsore Infection Complications
Understanding how untreated bedsores lead to serious infections.
Learn MoreGet Your Free Case Evaluation
Fill out the form below and our team will review your case immediately.
The information on this website is not legal advice. Contacting us does not create an attorney-client relationship. Past results do not guarantee future outcomes.